At Michigan Medicine, the standard goal for each call center is to answer at least 80 percent of inbound calls within 30 seconds. Meaning, each center strives to maintain an 80 percent service level and a sub-30-second average speed of answer (ASA). Although this standard had not been met for many years by the Radiology Call Center, the COVID-19 pandemic exasperated it even more.
From December 2019 to December 2020, the average Radiology ASA was 8:24 minutes with a service level of 22.33 percent and a call abandonment rate of 15.88 percent. Editor’s note: Data from March-May 2020 was excluded because of reduced operations during the COVID-19 pandemic. The worst performance was in September 2020 with an ASA of 20:30 minutes, a service level of 1.90 percent and an abandonment rate of 34.52 percent.
During the pandemic, one thing remained clear: The Radiology Call Center needed to improve patient access, and quickly.
 The Backstory
The Backstory
The Radiology Call Center schedules approximately 1,100 patients per day, requiring strict attention to detail for accuracy. Schedulers must consider protocols, diagnoses, key words, patient restrictions, contrast requirements, metal implants, patient weight and other factors when scheduling. These complexities led to call average handle times (AHT) ranging from 2 to 60 minutes, with an average of 8 minutes.
During March-April 2020, the pandemic was in full swing and Michigan in full lock-down, tensions were high and scheduling protocols were changing daily to adapt to the almost-hourly scheduling restriction updates. Michigan Medicine issued all call center agents equipment to work remotely. Prior to the work from home (WFH) mandate, working in the office was an option and the staff preference for remote work was about 50 percent. Fast forward four months and most agents wanted to continue working remotely and by January 2021, only one employee remained in the office because of the lack of high-speed internet access at home. While working remotely could have instilled fear in the employees, it was thankfully a first step in increasing the team’s morale and productivity.
In August 2020, leadership implemented a policy for “Performance Metrics Minimums.” These minimum expectations focused on three primary metrics:
- Average number of handled calls
- AHT
- Average wrap time to complete the call documentation.
To determine how each standard should be defined, individual agent metrics for a 13-month period were analyzed and compared to the team average for the same time frame. To encourage improvement, individual goals were set by improving those averages by about 5 percent each; the call volume standard was increased and the AHT and wrap time standards were decreased. This made the minimum expectations both reasonable and achievable.
Every month, call center leadership provided each agent with a report on their performance for the prior month and how those metrics compare to the team average. Within a few months, leadership noted three primary benefits:
- Top performing agents appreciated the recognition and are encouraged to continue performing well.
- Lower performing agents compared themselves to the average and are driven to improve their performance.
- All agents welcomed a defined set of expectations that ultimately instills a greater sense of accountability.
Until October 2020, the maximum staffing level was 26 representatives, which wasn’t enough to manage the daily average of inbound calls. Even with new performance patient access was still severely impacted; evidenced by a 30+ percent abandonment rate. And working in this environment was taking a toll on the agents, many spiraling towards burnout causing, reduced service levels, and lower morale. Due to budget restrictions, there were limited options for innovations or improvements.
The Results
After the first month of new standards, an average of six agents performed below the expected minimums. This trend improved by October 2020, with a steady average of one to two agents performing below the goal by April 2021. The improvement in performance created a domino effect on the overall call center performance statistics. Improved service levels were first noticed in October, when the ASA dropped from 20 minutes to 12 minutes and the abandonment rate from 34.52 percent to 22 percent. It was clear that the Radiology Call Center was finally heading in a positive direction.
While working from home, the agents’ reported reduced stress levels and improved work-life balance. The home environment made them feel more refreshed and happier about their work in general. And when employees feel positive about themselves and their work, their productivity and efficiency increases. In turn, the agents spread that positivity to each patient interaction.
Another testament to the increased job satisfaction was the reduction in voluntary turnover. Only two employees resigned within the first six months of the WFH mandate, one for retirement and one to accept a promotion. Previously, one agent per month on average would resign. Despite the improved work environment, call wait times were still averaging 20 minutes. Leadership’s next step was to look for ways to increase overall efficiency to maximize the available resources.
Even though the call center was trending in the right direction, service levels still did not meet Michigan Medicine standards and the barriers to patient access were potentially causing harm. Patients and clinics continued to complain and file reports on how difficult it was to schedule an exam. By November, the ASA was down to six minutes, but that still meant about half of the patients calling had long waits. Additionally, based on Erlang calculations, the call center was still short-staffed by six full-time employees. Given this data, the call center team obtained approval to increase staffing to the recommended levels despite the pandemic and financial recovery constraints.
To remain flexible, two of the incremental positions were posted as part-time flex positions. Those hired into these flex positions can work the days and shifts of their preference if they meet their 20 hours/week during normal operating hours. These two positions attracted more applications than the posting for four full-time positions. While interviewing, applicants made it clear that—in the environment created by COVID-19—having a job that is flexible and remote was more important than working full-time and earning more money. Posting these non-standard positions opened the applicant pool, increased call center flexibility, and supported the goal of employee satisfaction and work-life balance.
Due to space limitations, safety restrictions and trainer availability, leadership filled all open positions in two batches. Training averaged 4-6 weeks per agent, dependent on each person’s experience and learning ability. The first group completed training in January 2021, and the second completed training in early March. The impact to the ASA, service level and abandonment rate was immediate, and all metrics were soon exceeding the institution’s standards. The overall effectiveness of the additional staffing levels is depicted in the graphs shown. By April of 2021, the call center’s ASA was down to 8 seconds, the service level was up to 95.23 percent and the abandonment rate was a mere 0.28 percent!
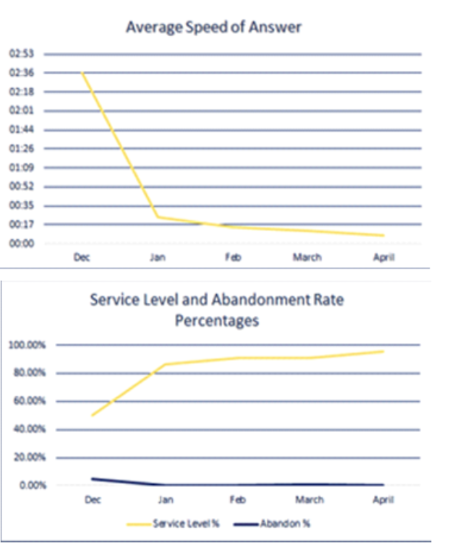
Additional changes have been made including streamlining internal processes and updating/clarifying staff resources. However, the greatest impact on employee satisfaction, and by extension patient access, was allowing the team to WFH, implementing performance standards and increasing staff. Although each initiative was different, together they resulted in increased team morale by reducing overall stress, spreading the workload more evenly and creating individual goals. When placed in a comfortable work environment and given the tools and the opportunity to be successful, employees are more likely to be productive, feel positive about their work and convey that positivity in each interaction with their patients.